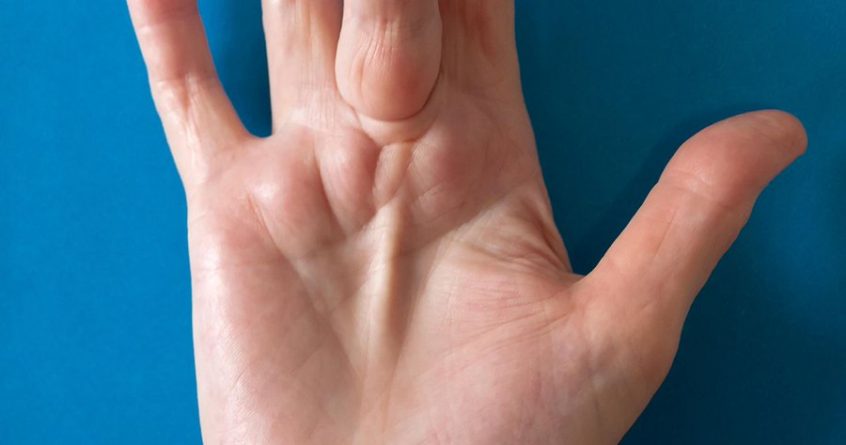
Have you ever heard of the condition Dupuytren’s contracture, which gradually causes the fingers to close in on the hand?
I was reminded of it by a recent report in the British Medical Journal, and a relative of mine had the condition so I could study it in detail and over time.
It’s estimated between 3% and 5% of people in the UK have DC. It starts as a thickening or pitting of the skin on the palm, then nodules appear and the fingers, usually the ring and little finger, get pulled in.
As Marta Karbowiak of Royal Surrey Community Hospital and colleagues explain in the BMJ, the exact cause of DC is unknown, though it runs in families in up to 80% of cases.
It’s more common in northern Europeans, with the highest rates in Nordic countries. It usually occurs at between 50 and 70 years old, and men are three times more likely to be affected.
As with most people, DC didn’t cause my relative much of a problem, and he never considered having surgery to correct it.
But if you do develop this condition, there are treatments out there to relieve it.
It’s worth mentioning that alcohol consumption and smoking have been linked to DC, and it can involve the feet (Ledderhose disease) and the penis (Peyronie’s disease).
Dupuytren’s disease is progressive and for some sufferers it can be severely debilitating, with patients experiencing considerable limitations at work and with everyday activities – such as putting on clothes and other manual tasks.
One treatment, percutaneous needle fasciotomy (PNF), divides the cord that has developed in the hand with a needle, and it can be done either as an outpatient or as a day case using local anaesthetic.
Recovery begins immediately with early hand exercises.
Most patients recover quickly and are able to return to normal daily activity within 10 days of the procedure.
However, recurrence of DC is common with this treatment, with half of people seeing a return after three years and 85% at five years.
Alternatively, surgical fasciotomy involves excision of the cord, but it has higher complication rates than PNF.
The most radical approach involves removing the entire portion of the diseased tissue. A surgeon will remove the skin, tendons and deep tissues of the hand, and it takes considerable time for the hand to heal.
While PNF results in better function and higher patient satisfaction after five weeks, surgery has a lower rate of recurrence.
In one Scandinavian study, only a third of patients had a recurrence of the contracture over an 18-year follow-up.