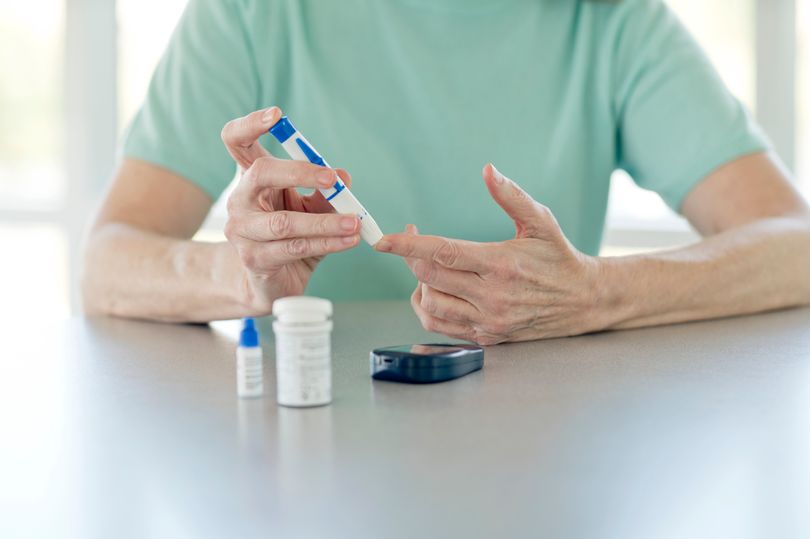
When I read about the stem cell treatment for diabetes from the Mayo Clinic I was reminded of an incident when I was a newly qualified doctor on A&E duty.
A middle-aged lady was brought in unconscious and smelling of alcohol.
“Another drunk!” was the verdict of the senior nurse.
Except it wasn’t alcohol, it was pear drops or acetone. This made me think “diabetes” and the lady was indeed in diabetic coma. But was it a ‘hypo’ or a ‘hyper’ – the treatment for each being very different?
The rule of thumb in these scenarios is to treat as hypo (low blood sugar) because this can cause brain damage. I asked for a large syringe of sugar solution and as I injected it into a vein the woman opened her eyes and asked for fish and chips! Relief all round.
It’s very different today. In what could be a step toward stem cell replacement therapy for diabetes, Mayo Clinic researchers have discovered how to repurpose stem cells to make the hormone that regulates low blood sugar, glucagon.
The Mayo Clinic research in the US, led by scientist Quinn Peterson, has come up with a new method of mass producing a stem cell treatment that’s capable of protecting diabetics against the hypoglycaemia that my patient in the A&E suffered from so long ago.
Normally we’re shielded from hypoglycaemia by the hormone produced in the pancreas called glucagon. It’s made by alpha cells but in diabetes these can stop working, leaving people susceptible to hypo- glycaemia.
“We now have the ability to manufacture large quantities of an important cell type that is necessary to prevent hypoglycaemia and regulate blood glucose in patients with diabetes,” says Dr Peterson.
“Generating pancreatic cell types from renewable sources holds promise for cell replacement therapies for diabetes.”
Stem cells can convert into alpha cells producing glucagon. When transplanted into animals, Dr Peterson’s team discovered these cells prevented hypoglycaemia.
According to Susan Buckles, Senior Communications Specialist at Mayo Clinic, researchers hope someday these cells could repopulate the pancreases of diabetics with glucagon-producing cells and the Mayo Clinic, through its Centre for Regenerative Medicine, could manufacture them.
“If successfully introduced into clinical use, these cells could dramatically change patient care for diabetes,” adds Dr Peterson.
“Rather than rely on routine blood checks to prevent hypoglycaemia and emergency room interventions to treat severe hypoglycaemia, in the future patients may be able to receive a transplant of living medicine that will both monitor blood glucose levels and administer corrective doses of glucagon.”
Clinical trials could start by 2022.